Modeling CAR T Cell Trafficking and Efficacy in Solid Tumors Using a Tumor–Vasculature-on-Chip
.avif)

Why This Is Important

Challenges

Need
MIMETAS’ Answer
A Tumor-on-a-Chip Model
Solid tumors remain a major challenge for CAR T cell therapy due to limited infiltration, heterogeneous antigen expression, and therapy-induced toxicity. To study how CAR T cells reach and engage solid tumors, MIMETAS scientists developed an on-chip model to evaluate CAR T cell migration and killing capacity. ECM-embedded colorectal cancer (CRC) cells were incorporated into a model comprising endothelium and T cells. CAR T cells were perfused through the human endothelial vessel adjacent to ECM-embedded tumor cells (Figure 1).
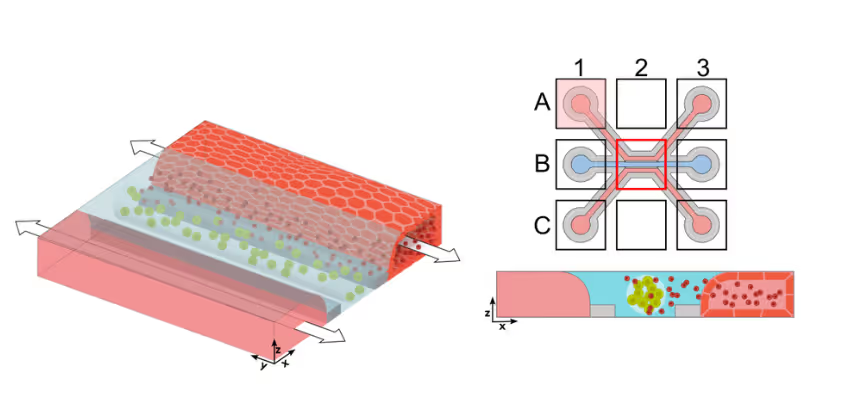
Figure 1. Schematic representation of the co-culture set-up. CAR T cells (red) are perfused through the endothelial vessel (light blue) via addition to the perfusion inlet (A1). Upon addition, CAR T cells adhere to the endothelial vessel wall and infiltrate the tumor compartment after undergoing the process of transendothelial migration.
CAR T Cell Trafficking to Tumor Compartment
CAR T cells were perfused through a human endothelial vessel adjacent to ECM-embedded tumor cells, enabling assessment of vascular adhesion, transendothelial migration, and tumor infiltration. CAR T cell infiltration increased over time and was strongly enhanced by a CXCL12 chemokine gradient, indicating active and directed migration (Figure 2A). CAR T cells infiltrated both target and non-target tumor cell compartments. Quantitative analysis revealed distinct infiltration dynamics between these conditions, with differences in the fraction of CAR T cells entering the tumor compartment over time (Figure 2B). These results demonstrate that CAR T cell trafficking is influenced by tumor context and is not solely determined by target recognition.
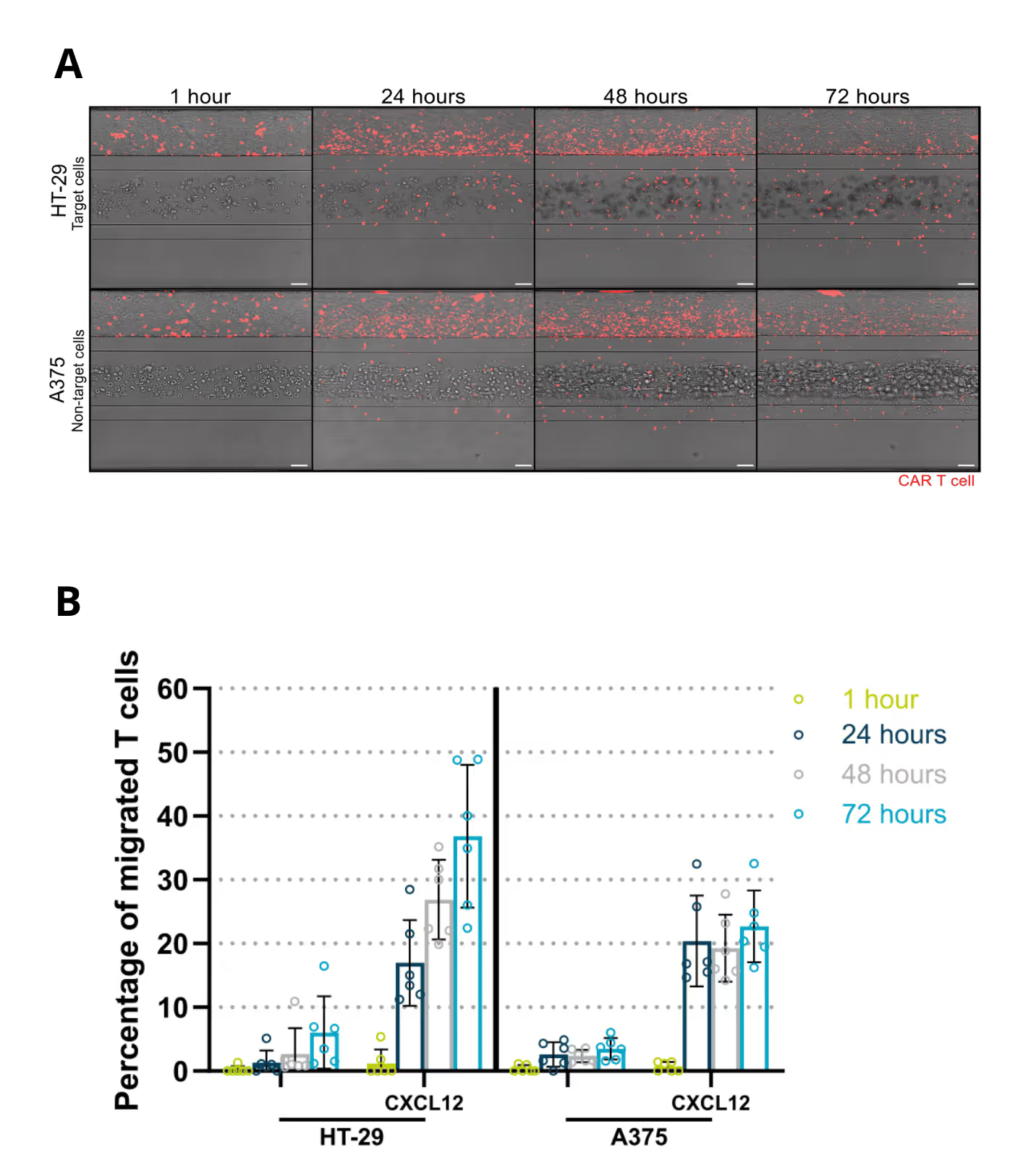
Figure 2. (A) Migration of fluorescently labelled CAR T cells towards target and non-target tumor compartments in the presence of a CXCL12 gradient over 72 hours of co-culture. (B) Percentage of migrated CAR T cells during 72 hours of co-culture with either target (HT-29) or non-target (A375) tumor cells.
Solid Tumor Killing by CAR T Cells
The colon organoid tubules recapitulate multiple essential epithelial functions. Upon exposure to vitamin D₃, gut cells show strong upregulation of CYP3A4, resulting in increased metabolic activity (Figure 3A). In addition, correct cellular polarisation and reporter expression enable highly reliable and physiologically relevant compound transport across the gut barrier (Figure 3B).
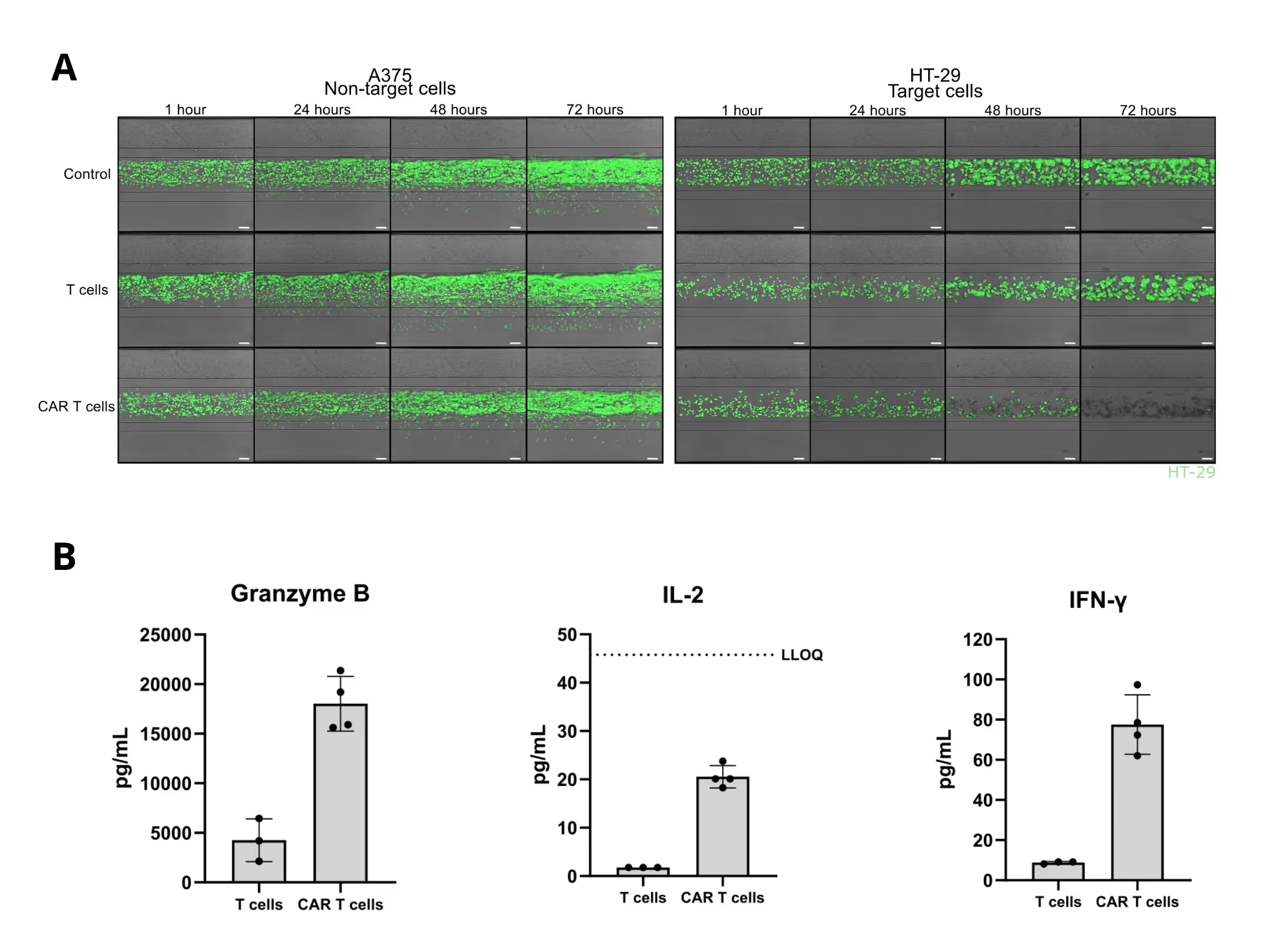
Figure 3. (A) Images of target and non-target tumor cells co-cultured with untransduced T cells or CAR T cells for 72 hours. (B) Cytokine levels after 72 hours of co-culture of target tumor cells with either untransduced T cells or CAR T cells for 72 hours.
Killing Efficacy of CAR T cells depends on Dosing
CAR T cell efficacy in solid tumors was strongly dependent on dosing. By varying the ratio of CAR T cells to tumor cells, the model captured clear dose–response relationships in tumor killing over time. Lower CAR T cell doses resulted in partial growth suppression of antigen-expressing tumor cells, whereas higher doses led to pronounced and sustained tumor clearance (Figure 4A).
Time-resolved imaging revealed progressive tumor cell loss with increasing CAR T cell dose, while quantitative analysis confirmed a strong, dose-dependent reduction in tumor area over 72 hours. These results demonstrate how the tumor–vasculature-on-chip model enables precise evaluation of CAR T cell dosing effects within a human-relevant 3D tumor microenvironment (Figure 4B).
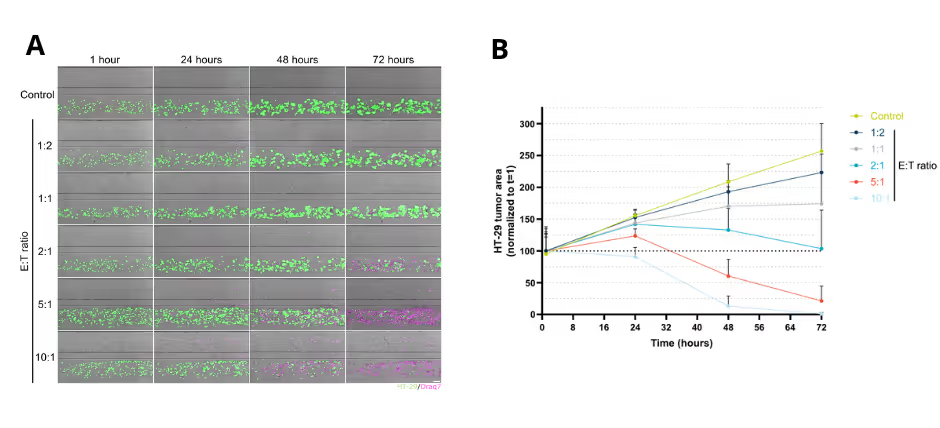
Figure 4. (A) Representative time-course images illustrating increasing tumor cell killing with higher CAR T cell doses. Draq7 signal indicates dead cells. (B) Quantitative analysis of tumor area over time demonstrates a clear dose–response relationship between CAR T cell dosing and tumor clearance.
Summary
- Simulation of Solid Tumor Microenvironment: Inclusion of factors such as immunosuppressive cells, soluble factors, and ECM stiffness.
- Accurate Immune Modeling: Real-time T-cell migration, engagement and cytokine release.
- Effective Construct Testing: Compare efficacy, and targeting precision of CAR T variants
References
- Chen Y, E C-Y, Gong Z-W, Liu S, Wang Z-X, Yang Y-S, et al. Chimeric antigen receptorengineered T-cell therapy for liver cancer. Hepatobiliary & Pancreatic Diseases International. 2018 Aug;17(4):301–9. doi:10.1016/j.hbpd.2018.05.005
- Siddiqui RS, Sardar M. A systematic review of the role of chimeric antigen receptor T (CAR-T) cell therapy in the treatment of solid tumors. Cureus. 2021 Apr 15; doi:10.7759/cureus.14494
Selected Resources
.avif)

.svg)




